When Red and Irritated Doesn't Mean Acne
Your client's skin is red, irritated, and breaking out. Your instinct says acne -- reach for the salicylic acid, schedule a peel, maybe add a retinoid to their home care. But what if the breakouts are not acne at all? What if the real problem is a damaged skin barrier -- and your next treatment is about to make it worse?
This is one of the most consequential judgment calls in esthetics. Getting it wrong means escalating the very condition you are trying to fix. Getting it right -- recognizing barrier compromise, pausing aggressive treatment, and repairing the foundation first -- is what separates estheticians who get lasting results from those whose clients cycle through the same frustrating pattern for months.
What the Skin Barrier Actually Does
Think of the skin barrier as a brick wall. The corneocytes -- dead skin cells on the outermost layer -- are the bricks. The lipid bilayer between them -- made up of ceramides, cholesterol, and fatty acids in roughly equal proportions -- is the mortar. When this structure is intact, it does two critical jobs: it keeps moisture in, and it keeps irritants, allergens, and pathogens out.
When the barrier is compromised, both functions fail. Moisture escapes, leading to dehydration. Irritants penetrate more deeply, triggering inflammation. The skin becomes reactive to products it previously tolerated. And that inflammation? It triggers breakouts -- not because the client has an acne condition, but because the barrier cannot do its job.
This is the overlap that confuses so many practitioners. The breakouts are real. The redness is real. But the root cause is structural damage, not clogged pores or excess sebum production. Treating it as acne with more acids and actives is like scrubbing harder at a wall that is already crumbling.
A compromised barrier does not need stronger products. It needs time, protection, and the right repair ingredients. Everything else comes after.
How to Tell the Difference
The challenge is that barrier damage and acne can look similar at first glance -- both involve redness, bumps, and unhappy skin. But the details tell a different story.
Signs That Point to Acne
- Comedones (blackheads and whiteheads) are present
- Pustules or cysts appear in consistent patterns -- along the jawline, on the chin, across the T-zone
- The breakout pattern is consistent over time, not sudden
- Skin tolerates products normally between breakouts
- Lesions are localized rather than spread across the entire face
Signs That Point to Barrier Damage
- Diffuse redness across broad areas, not limited to breakout zones
- Stinging or burning when applying products the client previously tolerated
- Skin feels tight and dehydrated but also produces excess oil -- the classic "dry but oily" complaint
- Sudden onset that correlates with product changes, new actives, or recent aggressive treatments
- Rough, flaky texture alongside breakouts
- The skin looks generally irritated rather than presenting distinct acne lesions
The Overlap You Need to Watch For
Here is the complication: a damaged barrier causes inflammatory breakouts that genuinely look like acne. The inflammation from barrier compromise can trigger pustules and papules that are clinically indistinguishable from inflammatory acne at first glance. The difference is in the history and context.
Ask your client: When did this start? Did you recently change products or add new actives? Have you been using more exfoliants than usual? Did another practitioner perform an aggressive treatment recently? If the breakouts coincide with increased active use or a recent peel, barrier damage is the more likely culprit -- even if the breakouts themselves look like acne.
Common Causes of Barrier Damage in Esthetics
Barrier damage in your clients is often iatrogenic -- meaning it was caused or worsened by the treatments and products that were supposed to help. Recognizing these causes is the first step to preventing them.
Over-Exfoliation
This is the most common cause. Daily AHA use combined with a retinol serum, plus enzyme masks once a week, plus professional peels every two weeks -- the math does not work. Each of these is fine in moderation. Stacked together, they strip the lipid barrier faster than the skin can rebuild it. The skin needs time between exfoliating treatments to repair itself. When you do not give it that time, the barrier thins and inflammation takes over.
Harsh Surfactants
Cleansers containing sodium lauryl sulfate (SLS) or sodium laureth sulfate (SLES) can strip the lipid matrix with every wash. For clients with already sensitized skin, this daily disruption prevents the barrier from ever fully recovering. A gentle, non-foaming cleanser is not a luxury recommendation -- it is a clinical necessity for compromised skin.
Too Many Actives, Too Fast
Introducing multiple active ingredients simultaneously -- niacinamide, vitamin C, retinol, AHA, and a peptide serum all in the first month -- overwhelms the skin. Even beneficial ingredients can cause irritation if the skin is not given time to acclimate. The enthusiasm to help can become the thing that harms.
Insufficient Recovery Between Professional Treatments
A chemical peel requires recovery time. If a client returns for another aggressive treatment before the skin has fully healed from the last one, you are compounding damage. Professional treatments should be spaced based on the skin's actual recovery, not the calendar availability.
Repair Protocol Basics
When you identify barrier damage -- whether it is the primary issue or a complicating factor alongside acne -- the repair protocol is straightforward in concept, even if it requires patience in practice.
Step 1: Strip Back Actives
Remove all exfoliating acids, retinoids, and aggressive actives from the client's routine. This includes professional treatments. Yes, this means pausing the acne protocol. If the barrier is compromised, nothing you layer on top will work as intended -- and much of it will make things worse.
Step 2: Simplify to Three Steps
The temporary routine should be: gentle cleanser, barrier-repair moisturizer, and broad-spectrum SPF. That is it. The cleanser should be non-foaming and free of sulfates. The moisturizer should contain barrier-repair ingredients. The SPF protects the compromised skin from UV-induced inflammation.
Step 3: Focus on Repair Ingredients
The ingredients that rebuild the lipid barrier are well-established:
- Ceramides -- the primary component of the lipid matrix. Topical ceramides help rebuild the "mortar" between skin cells.
- Niacinamide (2-5%) -- strengthens the barrier, reduces transepidermal water loss, and has anti-inflammatory properties. This is one of the few actives that is safe to use on compromised skin.
- Centella asiatica -- calms inflammation and supports wound healing. Look for formulations with madecassoside or asiaticoside.
- Squalane -- a lightweight lipid that mimics the skin's natural oils and helps restore the moisture barrier without clogging pores.
- Azelaic acid (low percentage) -- gentle enough for compromised skin and helps with both inflammation and any residual breakouts during repair.
Step 4: Wait
Barrier repair takes two to four weeks in healthy skin. If the barrier is severely compromised -- from months of over-treatment or particularly aggressive protocols -- recovery can take six to eight weeks. This is the hardest part. Both you and the client want to see active progress. But repair is active progress, even if it does not look dramatic. Document the changes at each visit so you can show the client that redness is fading, sensitivity is decreasing, and hydration is improving.
Step 5: Reintroduce Actives Gradually
Once barrier function is restored -- the skin tolerates products without stinging, redness has subsided, and hydration levels are stable -- you can begin reintroducing targeted acne treatments at lower concentrations and slower intervals. One new active at a time. Monitor for two weeks before adding anything else.
Barrier repair is not a detour from acne treatment. It is the prerequisite. Skipping it means every product and treatment you apply works against a foundation that cannot support it.
Why This Matters for Your Business
The clinical skill of distinguishing barrier damage from acne is also a powerful business differentiator.
Clients who come to you with damaged skin from other providers become your most loyal clients when you fix what others caused. The esthetician who pauses, explains what is actually happening, and takes a barrier-first approach earns trust that no discount or membership can replicate. These clients refer friends, write reviews, and stay for years.
Positioning yourself as a barrier-health-conscious practitioner also sets you apart from treatment-mill spas that push aggressive protocols on every client. In a market where many practitioners compete on the intensity of their treatments ("the strongest peel," "maximum extractions"), taking the opposite approach -- precision, patience, and protection -- attracts clients who are serious about their skin and tired of being over-treated.
The key to proving this approach works is documentation. When you can show a client their progress from session one (compromised, red, reactive) to session six (calm, hydrated, clear), the evidence speaks for itself. Use Skin SOAP notes to document barrier health at each visit -- transepidermal water loss observations, sensitivity responses, product tolerance, and visual changes. Over four to six sessions, the data tells a story that memory alone cannot.
Building a Barrier-First Practice
Making barrier assessment a standard part of your intake process is simpler than it sounds. Add barrier health as a category in every skin analysis. Note whether the skin shows signs of compromise before planning any treatment. When it does, lead with repair -- even if the client came in asking for an acne facial.
This shift doesn't slow you down. It makes your results predictable.
Why Most Barrier Repair Plans Fail (Even When You're Right)
You identified the barrier damage correctly. You gave the right instructions. You adjusted the protocol. And two weeks later, the client is still not improving.
Not because your plan was wrong. Because the execution was not consistent.
You are relying on memory. Scattered notes. What the client thinks they did at home. Barrier repair is not a single decision – it is a 4–8 week process that requires tracking, adjustments, and precise timing. Without structure, even the right plan falls apart.
Structure Is What Makes Precision Repeatable
When you can track barrier recovery session by session – document product tolerance, note sensitivity responses, and map out a phased repair plan – you stop guessing.
You know when to hold. You know when to adjust. And you know exactly when the skin is ready to move forward.
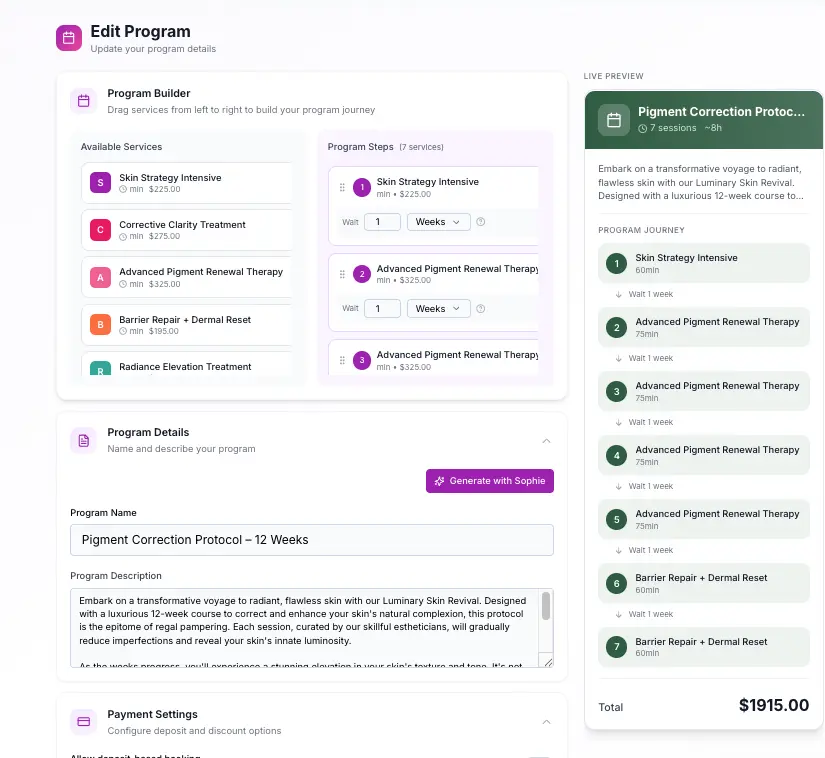 Map the full repair journey so every session builds on the last – not starts over.
Map the full repair journey so every session builds on the last – not starts over.
SpaSphere gives you that structure – combining Skin SOAP notes, client history, and treatment plans into one continuous timeline. So you are not treating based on memory. You are treating based on data.
Still tracking barrier recovery in your head? Build structured repair treatment plans with built-in documentation and see exactly when clients are ready to progress.



